What Is Squamous Cell Carcinoma?
Reviewed by: HU Medical Review Board | Last reviewed: May 2017. | Last updated: February 2023
Squamous cell carcinoma (SCC) develops in the flat cells that make up the outermost layer of skin. It is a non-melanoma skin cancer. Over 700,000 estimated new cases of SCC are diagnosed in the United States each year.1 SCC is less common than basal cell carcinoma (BCC), the other major type of non-melanoma skin cancer.
SCC tumors are typically on parts of the body that get the most sun exposure: face, ears, neck, lips, and back of the hand or forearm.2Rare locations for SCC include nails, vulva, and anus. People with fair skin, blue eyes, and red or light-colored hair who burn rather than tan are at the greatest risk of SCC.3 SCC is uncommon before age 50 years.3 If you have been diagnosed with one skin cancer, your risk of developing another one is much higher.
Can squamous cell carcinoma be cured?
The majority of SCC tumors are found early and treated while they are still small. Treatment at an early stage can usually remove SCC.2
SCC is more likely than BCC to invade deeper layers of skin and spread to other parts of the body.2 This is uncommon. However, about 5% to 10% of SCC tumors are considered “aggressive.”2,4 It is more difficult to treat aggressive SCC. By one estimate, between 3,900 and 8,800 white individuals died from SCC in 2012.1 In the Midwest and southern United States, SCC may cause as many deaths as melanoma.1
Your dermatologist may recommend regular follow up for several years after treating any SCC. Most (70% to 80%) of the cases that return (recur) do so with 2 years of initial treatment.5
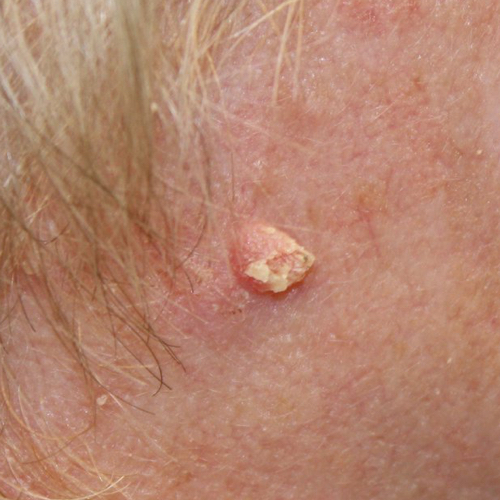
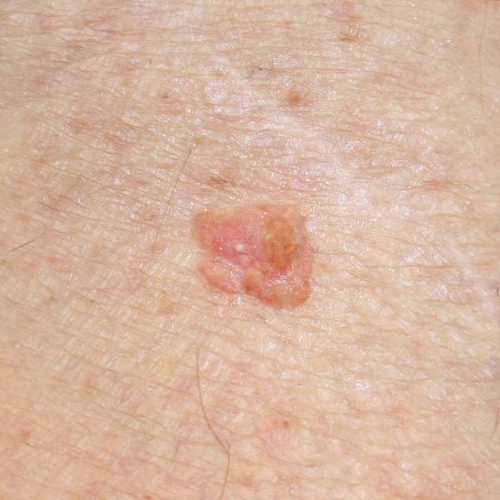
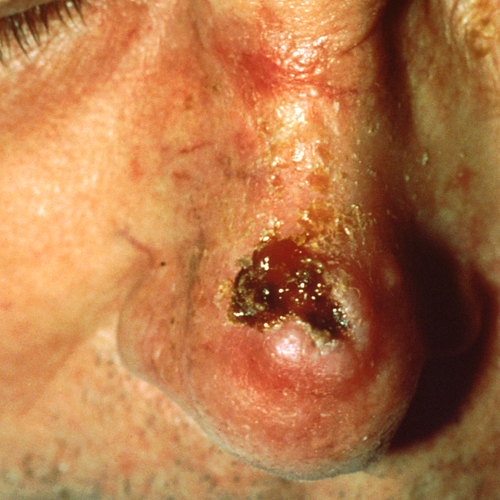
What does squamous cell carcinoma look like?
SCC may look like a firm, smooth bump, often with a depression or ulcer in the middle.3,6-8 It also can appear as a flat reddish or brownish patch.6 The lesion may be crusty or may bleed easily.
There are different forms of SCC and several precancers (abnormalities) that can lead to SCC:
Actinic keratosis:Actinic keratosis is a precancer that forms when cells in the top layer of skin (epidermis) begin to grow abnormally. About 6% to 10% of actinic keratoses grow into the dermis layer of skin and become SCC.3 Local treatment is able to address most actinic keratoses.
Bowen disease: Bowen disease is also called “squamous cell carcinoma in situ.” It is an early form of SCC. At this stage of disease, the cancer cells are only in the epidermis. These lesions are usually larger than actinic keratoses.
Keratoacanthomas: Keratoacanthomas are tumors that grow on sun-exposed skin. Some go away on their own. Others grow and spread. There is no way to predict what will happen, so they are usually treated as SCC. However, experts debate whether they are a form of skin cancer or if they are benign (harmless).2,3
Experts recommend regularly performing a skin self-examination.2Self-examination will help you to become familiar with your moles, freckles, and blemishes. Therefore, you will be able to identify changes in their size, shape, or color. Skin examinations by a doctor are not routinely recommended, but they may be important for people at a high risk of skin cancer. Ask your doctor how often you should have a total body skin exam.
What is aggressive squamous cell carcinoma?
“Aggressive SCC” or “high-risk SCC” is cancer that is more likely to recur (return after initial treatment) or metastasize (spread to other parts of the body). Features of high-risk SCC are:4,9
- Larger than 2 centimeters (cm)
- Deeper than 2 millimeters (mm)
- Near the lip and ear
- Located in a scar or other injured skin
- Spread into a nerve
- Poorly differentiated (abnormal cells and tissue structure)
Having a weakened immune system due to medications or infections increases the risk of aggressive SCC. History of radiation exposure or use of psoralen UVA treatment are other risk factors for aggressive SCC.9
How is squamous cell carcinoma treated?
The first choice of treatment for SCC is to remove the tumor.3 The specific type of surgery used depends on the tumor location and risk of recurrence.
Excision
A surgical knife is used to cut out (excise) the tumor. This technique may be used for tumors that are unlikely to return (recur). The area will heal rapidly, but the treatment will leave a scar.2,3
Mohs surgery
Mohs surgery is used to remove tumors that are large, invasive, or likely to return (recur).2,3 A specially trained surgeon removes a thin layer of skin and looks at it under a microscope. If the sample contains cancer cells, the surgeon removes another layer. This process continues until the sample contains no cancer cells.2 Mohs surgery is more expensive than other procedures. It has the highest success rates and saves the most healthy skin.2,3
Curettage and electrodesiccation
Curettage and electrodesiccation can be used to remove small SCC tumors. The doctor uses a long, thin instrument called a curette to scrape the cancerous tissue. The area is then treated with an electric needle, called an electrode, to destroy any remaining cancer cells. This surgery does not damage healthy skin. The treated area may heal slowly and scar.2,3
Radiation therapy
Radiation therapy is a treatment option when surgery is not possible or when the risk of recurrence is high. Cryotherapy can be used to treat actinic keratosis, Bowen disease, and small SCC.
Treatment options for advanced SCC are limited. Nearby lymph nodes may be surgically removed. This procedure is done to see whether there are cancer cells in the lymph nodes. Chemotherapy and immunotherapy may be used to treat SCC that has spread to distant parts of the body.
How can I prevent squamous cell carcinoma?
Sun protection
Ultraviolet (UV) light exposure is the most important modifiable risk factor for skin cancer. The risk of SCC has been linked to long-term sun exposure. This is the kind of sun exposure you might have if you have worked outside for many years.3,10 For this reason, SCC is rare in younger individuals.
Luckily, there are many ways to reduce your UV exposure, including:
- Using a broad spectrum sunscreen with sun protection factor (SPF) 15 or higher.
- Seeking shade between 10 am and 2 pm.
- Wearing long sleeves, long pants, wide-brimmed hats, and sunglasses.
- Avoiding indoor tanning beds.
Treat precancer
About 60% of SCC arises from actinic keratoses.3 For this reason, your doctor may recommend treating actinic keratosis.
Prevent HPV infection
Human papilloma viruses (HPV) are a group of viruses that can cause warts.2 Usually these warts are completely benign and do not lead to any type of cancer. However, some strains of this virus have been linked to SCC that develops in the genital and anal areas and around the fingernails. HPV can be spread through sexual contact. Safer sex practices include limiting sexual partners and wearing condoms. There is a vaccine against some HPV types.