What is Basal Cell Carcinoma?
Reviewed by: HU Medical Review Board | Last reviewed: May 2017. | Last updated: June 2020
Basal cell carcinoma (BCC) is the most common type of skin cancer — and the most common cancer overall.1,2 BCC develops in the top layer of skin, called the epidermis.2 BCC is most likely to develop on body parts that get the most exposure to sun: the head, the neck, and especially the nose.1,3,4 However, 1 in 3 tumors grow in areas that have little or no exposure to the sun.4
BCC is a non-melanoma skin cancer. The other major type of non-melanoma skin cancer is squamous cell carcinoma. The exact number of non-melanoma skin cancers is not known, because these cancers are not tracked in cancer registries. One estimate is that 5.4 million non-melanoma skin cancers are diagnosed each year in 3.3 million Americans, of which 80% are BCC.1,5
Having one incident of BCC puts you at risk for having another incident of BCC. One study showed that within one year after the first BCC, 33% of patients had one more BCC, 14% had two more, and 7% had three more BCCs.6
Is there a cure for basal cell carcinoma?
Yes, most cases of BCC can be cured. This type of cancer grows very slowly and almost never spreads to distant parts of the body (metastasizes).1,3,4 It is easiest to cure cancers when they are caught early.
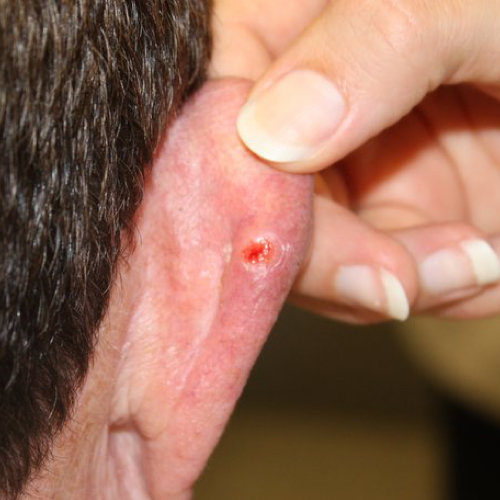
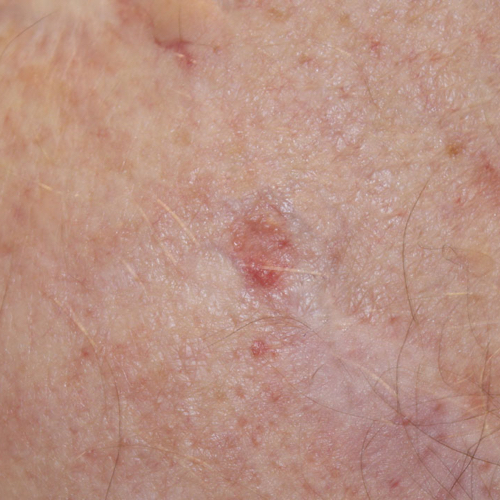
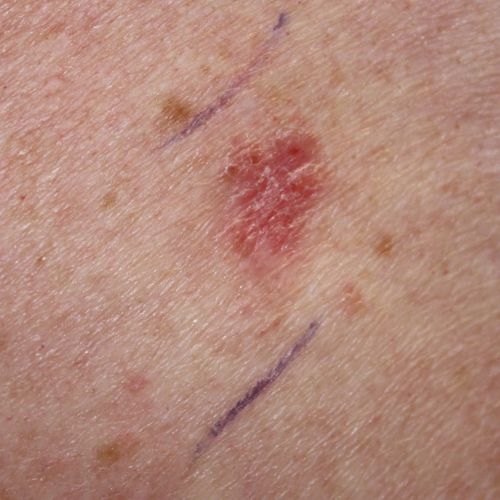
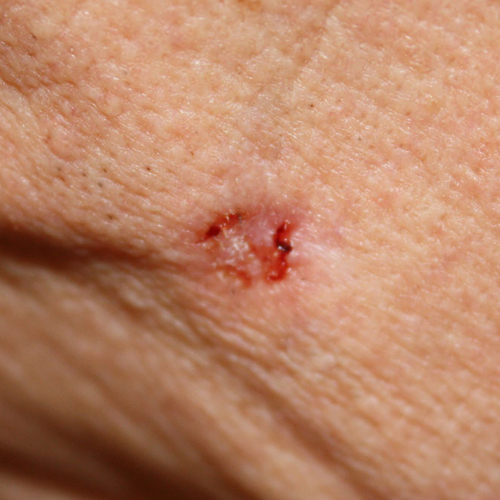
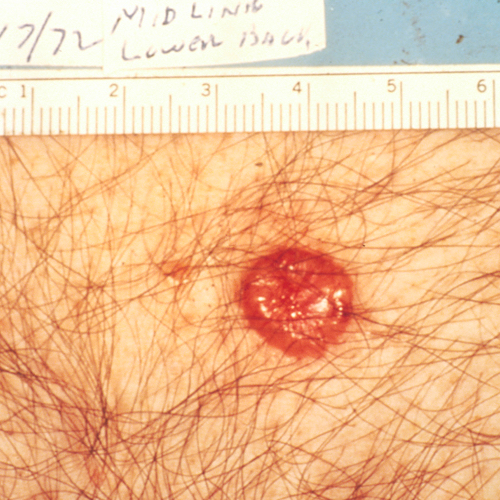
What does basal cell carcinoma look like?
BCC appears in many different ways.4,7,8 Discuss changes in your skin with your dermatologist. Experts recommend performing a skin self-examination regularly.1 This examination will help you to become familiar with your moles, freckles, and blemishes, so you will be able to identify changes in their size, shape, or color. Skin examinations by a doctor are not routinely recommended, but they may be important for people at a high risk of skin cancer. Ask your doctor how often you should have a skin examination.
What is complex basal cell carcinoma?
The terms “complex basal cell carcinoma” or “advanced basal cell carcinoma” are used to describe BCC with more aggressive features:9
- Growing into deeper layers of skin (invasive)
- Growing back after treatment (recurrent)
- Spreading to other parts of the body (metastasizing)
Abnormal feeling, such as pain or tingling, in the area can indicate aggressive BCC.10 These sensations could be a sign that the cancer has grown into a nerve. Cancers located around the nose, eyes, in front of the ears, or along the jaw line can be tricky to treat. Risks include loss of nerve function and possible deformity.10
Fortunately, such cases of BCC are rare. BCC is locally advanced in 0.8% of cases and metastatic in 0.04% of cases.9
What are treatments for basal cell carcinoma?
BCC is usually treated in the doctor’s office with relatively minor surgery.1 The specific type of surgery depends on the location of the tumor and likelihood of recurrence.
Excision
A surgical knife is used to cut out (excise) the tumor. This technique may be used for tumors that are unlikely to recur. The area will heal rapidly, but the treatment will leave a scar.1,4 About 5% of excised tumors recur within 5 years.4
Curettage and electrodesiccation
Another technique used for tumors that are unlikely to recur is curettage and electrodesiccation. Your doctor will remove the tumor using an instrument called a curette. The curette looks like a long, thin wand with a loop on the end that scrapes the tissue. Your doctor will treat the area with an electric needle, called an electrode, to destroy any cancer cells that remain. This type of surgery does not damage healthy skin. The treated area may heal slowly and scar.1,4 Between 8% and 18% of tumors treated with curettage and electrodesiccation recur within 5 years.4
Mohs surgery
When there is a greater risk that a tumor will recur, your doctor may remove it using a procedure called Mohs surgery. This surgery is expensive and must be done by a specially trained surgeon. It has the highest cure rates. Five years after Mohs surgery, only 1% of the tumors recur.4 It also saves the most healthy skin. This makes it good for cancers near the deye or cancers on the face, ear, or fingers. Mohs surgery is also performed when the tumors are large or invasive.1,4
To perform this surgery, your surgeon removes a thin layer of skin and looks at it under a microscope. If she or he sees cancer cells, then another layer will be removed. Your surgeon will continue to remove the skin one layer at a time until there are no cancer cells in the sample.
BCC is sometimes treated with other local therapies. Your doctor might recommend radiation therapy after surgery for tumors that recur or are highly likely to recur. If the tumor is very large or hard to treat surgically, radiation therapy can be used alone.1
Topical medications
Topical medications such as 5-fluorouracil and imiquimod may be used to treat cancers that are only in the very top layers of skin. However, it is more common to use topical medications to treat precancers.1,4
Cryotherapy
Cryotherapy, which involves freezing the lesion to kill cancer cells, is usually used to treat precancer. It is sometimes used to treat small, thin BCC.1
Targeted therapies
Targeted therapies may be used to treat patients with advanced or recurrent BCC. The two drugs approved for this use are Erivedge® (vismodegib) and Odomzo® (sonidegib).
How can I prevent basal cell carcinoma?
The most important modifiable risk factor for skin cancer is reducing ultraviolet (UV) light exposure. A few studies have linked intermittent, intense sun exposure during childhood and adolescence with developing BCC.2 This is the kind of sun exposure you might have during a summer day at the beach or pool. People who live close to the equator have more UV exposure and are more likely to develop BCC than people at higher latitudes.2Indoor tanning increases the risk of BCC by approximately 40%.2
Luckily, there are many ways to reduce your UV exposure, including:
- Using a broad spectrum sunscreen with sun protection factor (SPF) 15 or higher.
- Seeking shade between 10 am and 2 pm.
- Wearing long sleeves, long pants, wide-brimmed hats, and sunglasses.
- Avoiding indoor tanning beds.
There are other risk factors for BCC that you cannot change. These include light skin color, tendency to burn, freckling, medical history, age, and gender. People at high risk of skin cancer can take steps to detect cancer early when it is easiest to treat.